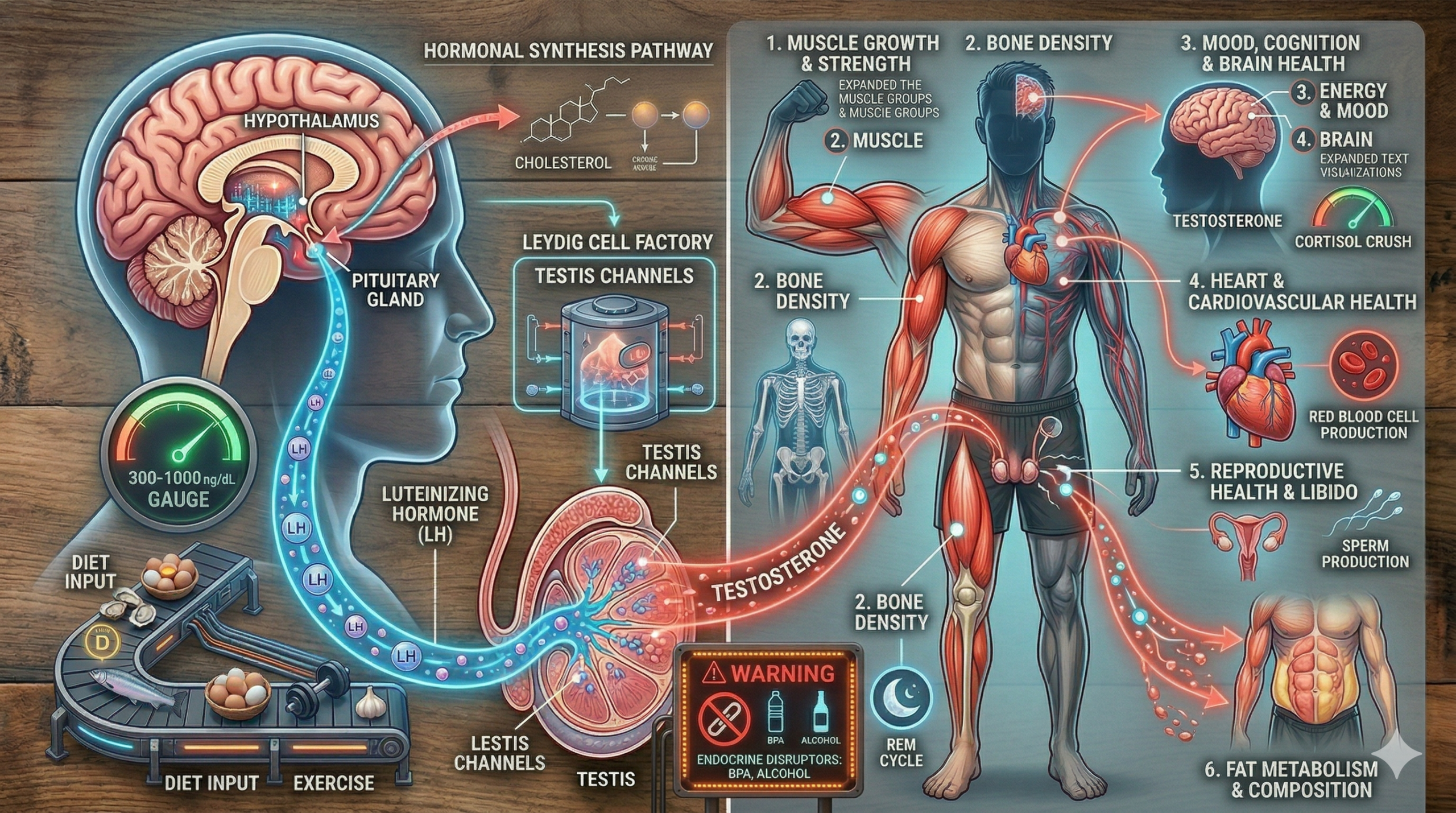
What does testosterone actually do in the body?
Testosterone is the primary male sex hormone, but calling it purely male is misleading. Women produce it too, just in much smaller amounts. Like all hormones, testosterone functions as a chemical messenger: it travels through the bloodstream and tells cells and organs what to do. Its influence is broader than most people realize.
~7 mgDaily testosterone production in men
~0.7 mgDaily testosterone production in women
Age 30When natural decline typically begins
~1%Annual decline rate after age 30
Testosterone functions: men vs. women
In men, testosterone drives the development and maintenance of what most people associate with male biology. In women, it plays a supporting role in libido, bone health, and muscle tone, though at concentrations roughly ten times lower. Both sexes experience measurable effects when levels fall outside the healthy range.
Primary sexual characteristics and other roles testosterone plays
In men specifically, testosterone is responsible for the formation of primary sexual characteristics during development, ongoing sperm production throughout adult life, and the secondary characteristics that emerge at puberty: beard growth, chest and pubic hair, the voice-deepening process known as voice breaking, and potency.
Beyond reproduction and appearance, testosterone in the human body also regulates muscle development and bone density, drives the production of red blood cells (erythrocytes), governs fat metabolism, stabilizes mood and cognitive function, and sustains sexual desire and libido. This is why low testosterone rarely shows up as just one complaint; it touches nearly every system.
Secondary traits
Systemic
Mental health
Why testosterone levels fall
Some testosterone decline is natural and inevitable. But the speed and severity of that decline are significantly shaped by how you live. Understanding what suppresses testosterone production is the first step toward protecting it.
Testosterone decline with age — and the question of andropause
From around age 30 to 40, men steadily produce less testosterone. For many, this is so gradual that their levels remain within normal range well into retirement. For others, the drop is steeper and noticeable. This phenomenon, sometimes called andropause, male menopause, or climacterium virile, is real, but controversial in its clinical significance.
Unlike women, men don’t experience an abrupt hormonal drop. The decline is slow and diffuse, which is partly why about half of men going through it don’t notice anything at all. The ones who do tend to attribute symptoms to ageing in general rather than hormonal changes specifically. This is why andropause remains underdiagnosed and underestimated.
Testosterone decline with age is not a disease in itself. Whether it requires medical intervention depends on the degree of decline and whether it's causing symptoms that affect quality of life.
Lifestyle and medical causes of low testosterone
Beyond age, a number of factors actively accelerate the fall in testosterone levels. Some are lifestyle-driven and reversible. Others are medical and require clinical management.
Alcohol and its effect on testosterone
Frequent or heavy alcohol consumption directly impairs testosterone production. Alcohol damages the Leydig cells in the testes responsible for synthesis, disrupts the sleep quality that testosterone depends on, and elevates cortisol, itself a testosterone suppressor. Even moderate regular drinking has a measurable downward effect over time.
Stress, cortisol, and the testosterone connection
Chronic psychological stress triggers the sustained release of cortisol, the body’s primary stress hormone. Cortisol and testosterone are biological opposites in many respects: when one is chronically elevated, the other tends to be suppressed. Stress cortisol testosterone is not just a wellness cliché; it’s a documented hormonal mechanism.
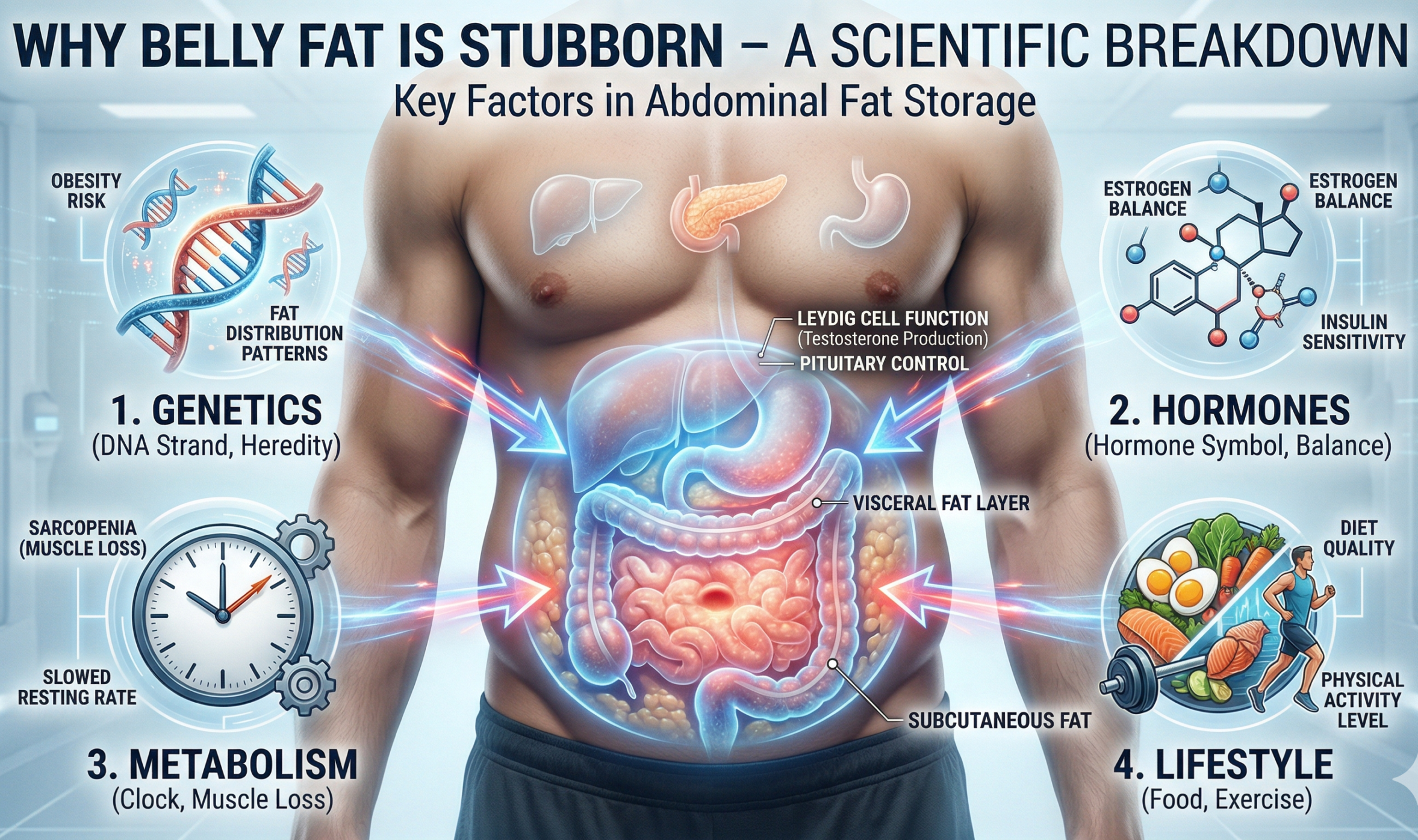
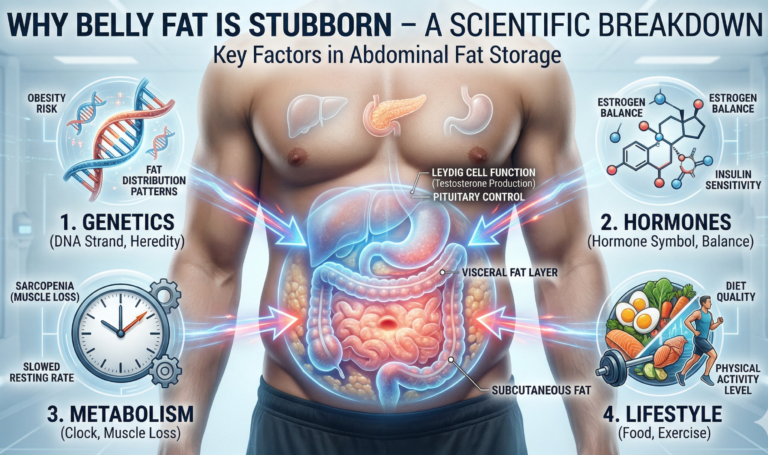
Abdominal fat, visceral fat, and estrogen conversion
Intra-abdominal fat — technically called visceral fat — is hormonally active tissue. It produces signaling molecules that inhibit testosterone production, and it triggers metabolic processes that convert testosterone into oestradiol, a female sex hormone. The result is a self-reinforcing cycle: low testosterone promotes fat accumulation, and that fat further reduces testosterone.
Chronic diseases that lower testosterone
Several medical conditions are associated with testosterone deficiency. Liver cirrhosis testosterone suppression occurs because the liver plays a key role in hormone metabolism. Renal insufficiency and testosterone decline are linked to the kidneys’ involvement in hormonal regulation. Type 2 diabetes testosterone deficiency is particularly well-documented; insulin resistance and poor metabolic health consistently correlate with low androgen levels. Metabolic syndrome testosterone suppression follows similar pathways. Certain cancers and severe malnutrition, including anorexia, also disrupt the hormonal balance in both men and women.
Medications that lower testosterone levels
Opioids testosterone suppression is one of the most clinically significant drug-related causes of low androgen levels, a known and often underappreciated side effect of long-term painkiller use. Corticosteroids, testosterone suppression, hormonal contraceptives, testosterone effects, and some antidepressants, testosterone interaction are all documented. If you’re on long-term medication and experiencing symptoms of low testosterone, a conversation with your prescribing doctor is worthwhile.
Never stop prescription medication to try to improve testosterone levels without medical guidance. Many of the medications involved treat serious conditions, and the risk of stopping them outweighs the benefit of any hormonal improvement.
Symptoms and consequences of testosterone deficiency
Low testosterone rarely announces itself clearly. The symptoms are non-specific, which means they overlap with many other conditions and are often dismissed as signs of normal ageing or stress. Recognizing the pattern matters.
Symptoms of testosterone deficiency in men
General symptoms that can appear regardless of age or sex include persistent fatigue, loss of performance, low motivation, depressive mood, and difficulty concentrating. Physical changes include declining bone density and muscle mass alongside increases in abdominal fat.
In men who are past puberty, testosterone deficiency may also present as:
Diseases and conditions linked to testosterone deficiency
Left unaddressed over time, low testosterone isn’t just uncomfortable — it raises the risk of serious conditions. The link between diabetes and testosterone is well-established: low testosterone worsens insulin resistance, and insulin resistance further suppresses testosterone. The osteoporosis testosterone connection is direct — bone density depends on adequate androgen signaling. Arterial calcification and testosterone reflect the cardiovascular role testosterone plays in vascular health. Anemia testosterone deficiency occurs because testosterone stimulates erythrocyte production — without enough of it, red blood cell counts can fall.
How to increase testosterone naturally
The good news is that testosterone levels are not entirely fixed. For most people, a combination of dietary changes, targeted supplementation, exercise, and lifestyle adjustments can produce real, measurable improvements — especially when levels have been suppressed by modifiable factors.
A testosterone-boosting diet: what to eat and what to avoid
Diet is the most accessible lever most people have for supporting natural testosterone production. The goal isn’t a rigid meal plan — it’s shifting the overall nutritional pattern in a direction that supports hormone balance.
Healthy fats are the foundation
Testosterone is synthesized from cholesterol, which means dietary fat is a prerequisite for hormone production. The key is fat quality. Healthy fats from eggs, nuts, seeds, and plant oils — sources rich in monounsaturated and polyunsaturated fatty acids — provide the raw materials for testosterone synthesis without the cardiovascular downsides of saturated fat excess.
Eggs, Almonds, Walnuts, Pumpkin seeds, Olive oil, Avocado, Flaxseed
Low sugar, low white flour — insulin and testosterone are linked
High-glycemic foods cause rapid spikes in blood sugar, which trigger large insulin releases. Elevated insulin directly suppresses testosterone. On top of that, excess sugar is stored as body fat — particularly abdominal fat — which then converts testosterone to estrogen. A low sugar diet for testosterone isn’t about eliminating carbohydrates; it’s about choosing the right ones.
Foods to reduce or avoid
- Sweets, pastries, biscuits, and confectionery
- White bread, white pasta, white rice, and refined white flour products
- Fruit juices, smoothies, and sugary soft drinks
- Processed snack foods with added sugar
Fiber-rich foods stabilize blood sugar and support testosterone
Fiber slows the absorption of sugar into the bloodstream, preventing the insulin spikes that suppress testosterone. Legumes, fruits, vegetables, and whole grains are the primary fiber sources — and the research on fiber foods testosterone connection is consistent: higher fiber intake correlates with better hormonal health. These foods also support gut health, which influences systemic inflammation — another testosterone suppressor.
Avoid alcohol — or at least limit it meaningfully
A drink on a special occasion is unlikely to cause measurable harm. Regular or heavy consumption is another matter entirely. The advice here isn’t abstinence for everyone — it’s awareness that alcohol avoidance testosterone benefits are real, and that even moderate regular drinking creates a background hormonal drag over time.
What about the Mediterranean diet?
The Mediterranean dietary pattern — rich in vegetables, legumes, whole grains, healthy fats, and lean protein — naturally incorporates all of these principles. It’s the most evidence-backed overall dietary framework for men’s hormonal health.
Natural supplements and home remedies for testosterone
Targeted supplements can fill gaps that diet alone may not address. The evidence varies by compound — some are well-supported, others are more limited. Here’s an honest look at the four most relevant ones.
A note on natural remedies and testosterone supplements
These supplements work best when there’s an underlying deficiency or imbalance to correct. Someone with adequate zinc, vitamin D, and low stress will see less benefit than someone deficient in one or more of these areas. Testing before supplementing — rather than supplementing blindly — is always the smarter approach.
Exercise and testosterone — what the evidence actually says
Sport and physical training are among the most powerful natural tools for boosting testosterone. Exercise increases testosterone directly by stimulating hormonal output from the testes. It also reduces cortisol levels, removing one of testosterone’s main biological suppressors.
Strength training for testosterone
Resistance training — particularly compound movements involving large muscle groups — produces the strongest acute testosterone response. Weight training testosterone benefits are well-established, both in the short term (testosterone spikes following a session) and over time (improved baseline hormonal output with consistent training). Squats, deadlifts, rows, and presses are more effective than isolated exercises.
Endurance training — benefits and limits
Endurance training testosterone support is real but more modest than resistance training. Cardio improves cardiovascular health, reduces visceral fat, and lowers resting cortisol — all of which support testosterone indirectly. However, excessive endurance training flips this relationship. Hours of continuous running, especially without adequate recovery, elevate cortisol chronically and can actually suppress testosterone. This is why overtraining testosterone suppression is common among competitive endurance athletes.
The overtraining problem
More is not always better when it comes to testosterone. Training volume beyond what the body can recover from consistently raises cortisol and suppresses testosterone production. Two to four resistance sessions per week, with adequate rest between them, is the evidence-based target for most men.
Sleep, sexual activity, and lifestyle changes for testosterone
Diet and exercise get most of the attention in testosterone discussions, but sleep may be the single most underestimated factor of all.
Sleep and testosterone — the overnight production window
Most daily testosterone production happens during sleep, peaking during REM cycles. Sleep deficiency testosterone suppression is swift and measurable: a study showed that sleeping fewer than five hours a night significantly lowers testosterone levels in the blood. The mechanism is direct — sleep deprivation disrupts the nocturnal LH pulses that signal the testes to produce testosterone. Healthy sleep testosterone production requires both sufficient duration (7–8 hours) and quality — fragmented sleep that prevents proper REM cycling has similar effects to sleep deprivation.
Testosterone decline and sleep are real and reversible phenomena. Improving sleep quality and duration is one of the fastest-acting natural testosterone interventions available.
Sexual activity and testosterone
Men who are regularly sexually active tend to maintain higher testosterone levels. The relationship appears to be bidirectional — testosterone drives libido, and sexual activity in turn stimulates testosterone production. A full, active sex life is not just emotionally healthy; it appears to support the male hormonal axis.
Body weight, lifestyle, and aging gracefully
It is never too late to take action. Even in older men, the combination of a healthy diet, regular exercise, adequate sleep, healthy body weight, and targeted supplementation with zinc or ashwagandha can improve testosterone levels to a meaningful degree. The factors that matter for testosterone health at 40 are largely the same ones that matter at 70.
Testosterone reference values for men and women
Testosterone is measured via blood test — specifically from blood serum, though plasma, urine, and saliva testing are also possible. Two key metrics are typically assessed: total serum testosterone (the overall amount) and free testosterone (the biologically active fraction not bound to proteins).
Total serum testosterone — normal ranges
| Population | Normal range (μg/l) | Normal range (nmol/l) |
|---|---|---|
| Adult men | 3.5 – 9.0 | 12.1 – 31.2 |
| Adult women | 0.15 – 0.55 | 0.52 – 1.91 |
Free testosterone in serum — age-stratified reference ranges (men)
| Age group | Men (μg/l) | Women (μg/l) |
|---|---|---|
| 18 – 39 years | 8.8 – 27.0 | Up to 2.57 |
| 40 – 59 years | 7.2 – 23.0 | Up to 2.03 |
| 60 – 80 years | 5.6 – 19.0 | Up to 1.55 |
How to convert testosterone values
Laboratory results in μg/l can be converted to nmol/l by multiplying by 3.467. Always compare your result against the reference ranges provided by the specific laboratory that ran your test, as calibration methods vary between facilities.
What to do if your testosterone is low
A single low reading does not necessarily confirm a deficiency — testosterone fluctuates throughout the day, peaking in the morning. A second test, ideally taken in the morning, is standard practice before clinical conclusions are drawn. If confirmed low, a doctor will typically explore whether the cause is primary (testicular), secondary (pituitary/hypothalamic), or lifestyle-related, and recommend treatment accordingly.
Free testosterone is often more clinically meaningful than total testosterone. A man can have total testosterone in the normal range but still be functionally low if most of it is bound to proteins and unavailable for use by cells.
Frequently asked questions about increasing testosterone
What should I eat to increase testosterone levels?
Focus on whole, unprocessed foods: vegetables, legumes, fruits, and whole grains for fiber and micronutrients; eggs, nuts, seeds, and plant oils for healthy fats that support hormone synthesis. Reduce sugar, white flour products, and alcohol. There is no single testosterone superfood — the overall dietary pattern matters more than any individual ingredient.
What increases testosterone the most?
In practical terms, consistent resistance training, adequate sleep (7–8 hours), and reducing visceral fat have the most documented impact on naturally increasing testosterone. If a deficiency in zinc or vitamin D is present, correcting it can produce significant improvements. Ashwagandha is the best-supported supplement for direct testosterone stimulation.
Do onions increase testosterone?
There is preliminary research — primarily in animal studies — suggesting that onion juice may increase testosterone by stimulating LH production and reducing oxidative stress in the testes. Human evidence is limited. Onions are a valuable part of a testosterone-friendly diet, but don’t rely on them as a primary intervention.
What should I do if I have too little testosterone?
First, confirm it with a blood test — ideally two morning measurements. Then work through modifiable causes: sleep, exercise, diet, alcohol, stress, and body weight. If lifestyle changes don’t move the needle and levels remain clinically low with symptoms, a doctor may consider testosterone replacement therapy or other medical interventions. Self-diagnosis and self-treatment without testing first is not advisable.
Can women benefit from naturally increasing testosterone?
Yes. Women with low testosterone may experience fatigue, reduced libido, muscle weakness, and mood issues. The same lifestyle factors — adequate sleep, resistance training, healthy diet, stress management — support healthy testosterone in women. Medical intervention requires more care in women due to the narrower therapeutic range, so specialist input is particularly important.