If you’ve been feeling tired for no clear reason, losing muscle even though you haven’t changed your routine, or noticing your sex drive quietly disappear — you’re not imagining things. These are real symptoms, and for many men, they trace back to one root cause: low testosterone.
This guide breaks down everything you need to know, in plain language, without the medical jargon overload.
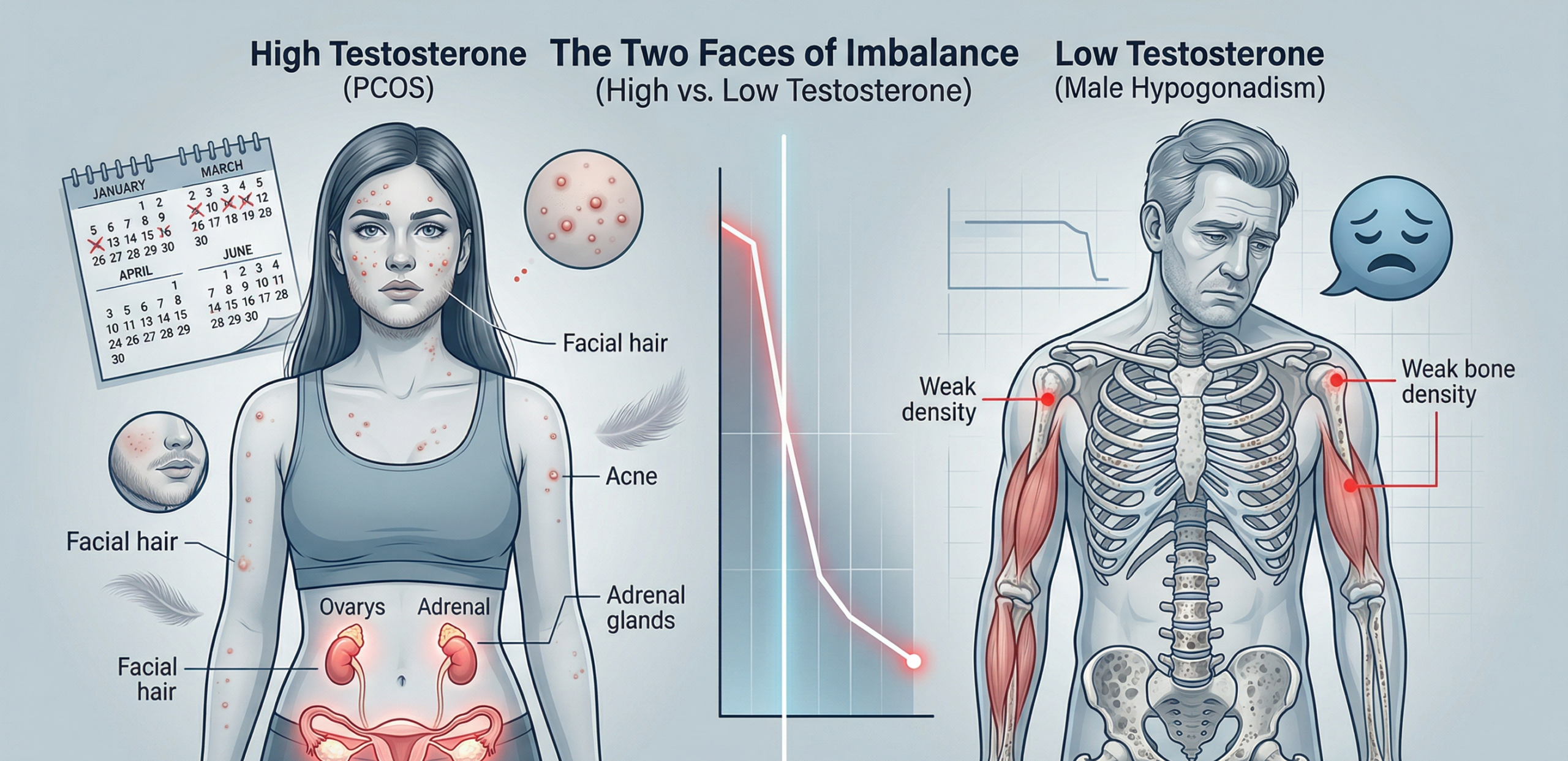
What Is Low Testosterone — And Why Does It Matter?
Testosterone is the primary male sex hormone, produced in the testicles. It drives puberty — the voice changes, the facial hair, the muscle development. Beyond adolescence, it continues to regulate sex drive, sperm production, bone strength, mood, and energy.
The problem is that testosterone levels naturally decline with age. That’s normal. But when levels fall below what the body needs to function properly, it becomes a medical condition — called Testosterone Deficiency Syndrome (TD), or more commonly, Low Testosterone (Low-T).
The American Urology Association (AUA) sets the clinical threshold at below 300 nanograms per deciliter (ng/dL). Fall below that, and your body starts sending signals — even if you don’t immediately recognize them as hormone-related.
How Common Is Low-T? More Than Most Men Realize
Roughly 2.1% of men overall have clinically low testosterone. That number sounds small until you break it down by age and health status:
- About 1% of younger men are affected
- Up to 50% of men over 80 may have Low-T
- 30% of overweight men tested low in one major study, compared to just 6.4% of men at normal weight
- 24.5% of men with diabetes had Low-T, versus 12.6% of those without
The takeaway: Low testosterone is far more common in men managing weight problems or metabolic conditions. If that’s you, it’s worth paying attention.
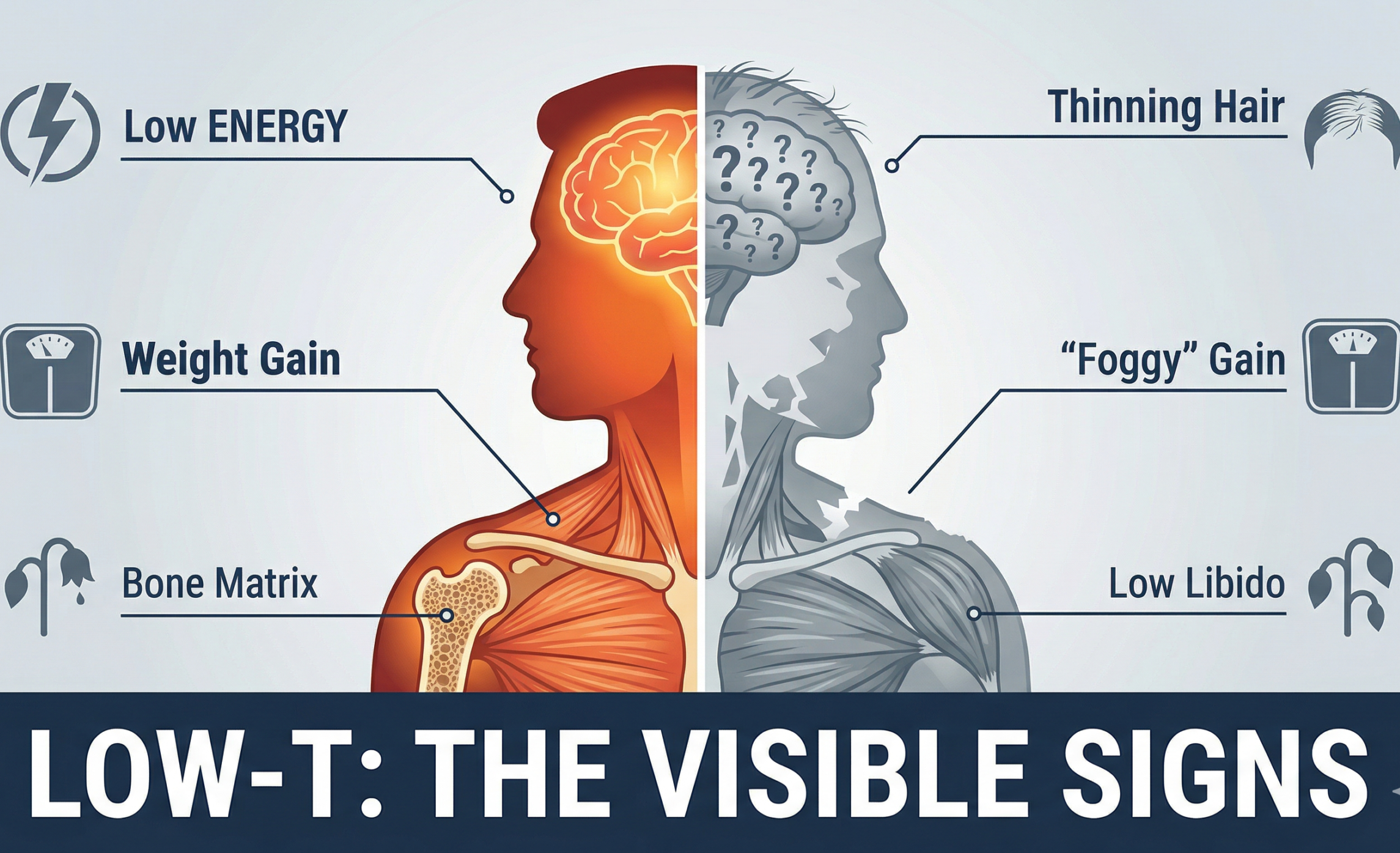
Low Testosterone Symptoms: What to Actually Watch For
Specific Symptoms Directly Linked to Low-T
These symptoms have a stronger, more direct connection to testosterone deficiency:
- Reduced sex drive
- Difficulty achieving or maintaining erections
- Loss of lean muscle mass
- Less body and facial hair
- Constant, unshakeable fatigue
- Weight gain, particularly around the belly
- Persistent low mood or depression
Non-Specific Symptoms That May Also Indicate Low-T
These are less definitive on their own, but worth noting if you’re also experiencing specific symptoms:
- Low energy and reduced physical endurance
- Poor memory or mental fog
- Struggling to find words mid-conversation
- Difficulty focusing
- Declining performance at work
One symptom alone rarely tells the full story. But if you’re dealing with a combination — say, fatigue, low sex drive, and emotional flatness all at once — that pattern is worth discussing with a doctor.
What Causes Low Testosterone?
Conditions You’re Born With
Some men are born with genetic conditions that affect testosterone production from the start:
- Klinefelter syndrome — the most commonly cited congenital cause
- Noonan syndrome
- Ambiguous genitalia development
Conditions That Develop Over Time
Others develop Low-T because of damage or disease:
- Testicular injury or surgical removal (often due to cancer)
- Chemotherapy or radiation
- Pituitary gland disorders
- Infections or autoimmune conditions
Lifestyle and Health-Related Causes
This category affects the most men and is also the most actionable:
- Aging — gradual, unavoidable, but manageable
- Obesity — one of the strongest modifiable risk factors
- Metabolic syndrome — the combination of high blood pressure, high blood sugar, poor cholesterol, and belly fat
- Certain medications — antidepressants and opioid pain medications both suppress testosterone
- HIV/AIDS — approximately 30–50% of men with these conditions also have Low-T
How Low Testosterone Is Diagnosed
Symptoms matter, but they aren’t enough on their own. A proper diagnosis requires blood work — specifically a total testosterone blood test, ideally taken twice before noon on separate occasions. Testosterone levels dip naturally later in the day and during illness, so timing the test correctly is important.
What Your Doctor Will Also Check
Beyond testosterone levels, expect your doctor to investigate:
Health history questions covering puberty development, head trauma, medication use (steroids, opioids, glucocorticoids), chemotherapy history, family history of Low-T, and prior heart attacks or strokes.
A physical examination assessing body weight and composition, hair distribution, breast tissue changes (gynecomastia), testicular presence and size, and prostate health.
Additional blood tests, including:
- Luteinizing hormone (LH) — to identify whether the problem originates in the brain or the testicles
- Prolactin levels — elevated prolactin can point to a pituitary tumor
- Hemoglobin — to assess anemia
- FSH (follicle-stimulating hormone) — relevant if fertility is a concern
- HbA1C — to screen for diabetes
- Estradiol — if breast symptoms are present
An MRI of the pituitary gland, bone density scans, or chromosomal testing may also be ordered depending on your individual situation.
Testosterone Therapy (TT): Who Needs It and What It Involves
Testosterone therapy is not a lifestyle upgrade for men who feel a bit sluggish. The AUA is explicit: TT should only be prescribed to men who meet both clinical and laboratory criteria — meaning confirmed symptoms and a blood testosterone level under 300 ng/dL.
Five Ways to Take Testosterone
There’s no universally “best” method. Each has practical trade-offs:
Transdermal (Gels, Creams, Patches) — Applied to dry skin daily. Effective, but topical forms can transfer to others. Wash your hands thoroughly. Keep children and women away from treated skin. Patches carry a lower transfer risk than gels or liquids.
Injections — Short-acting (weekly or bi-weekly) or long-acting (monthly). Given into the muscle. Efficient, but some men experience side reactions. Long-acting injections carry a rare but serious allergy risk — doctors monitor you in the office after administration.
Oral/Buccal Tablets — Placed against the upper gum near the canine tooth, not swallowed. Releases over 12 hours. Easier on the liver than swallowed testosterone, but can cause local irritation or headaches.
Intranasal Gel — Pumped into each nostril, typically three times daily. Straightforward but requires consistent timing throughout the day.
Subcutaneous Pellets — Implanted under the skin of the hip or buttocks under local anesthesia. Releases slowly over 3–6 months. Fewest daily requirements, but involves a minor procedure.
Your insurance provider may influence which option is available to you. It’s a practical conversation to have upfront.
Side Effects of Testosterone Therapy: What’s Real and What’s Overstated
Confirmed Side Effects
- Blood thickening (erythrocytosis) — TT raises hemoglobin and hematocrit levels, which can increase clotting risk. Doctors monitor this with blood tests 2–6 weeks after starting, then every 6–12 months.
- Reduced sperm production — TT is not compatible with active family planning. If children are in your near-term plans, discuss alternatives first.
- Skin reactions — Redness, itching, or rash at application or injection sites.
- Transfer risk from topical forms — Particularly concerning for children and women in your household.
What the Evidence Does NOT Support
- No proven link between TT and prostate cancer.
- No strong evidence that TT increases the risk of venous clots.
- No strong evidence that TT raises or lowers cardiovascular event risk — though the FDA still requires labeling about this possibility. If you have a history of heart disease, closer monitoring is standard practice.
What to Expect After Starting Treatment
Results don’t happen overnight. Most men notice changes within three to six months. Testosterone therapy has the strongest evidence for improving:
- Erectile function
- Sex drive
- Bone density
- Muscle mass
- Anemia
- Depressive symptoms
Where the evidence is weaker: energy levels, memory, lipid profiles, diabetes management, and general quality-of-life metrics. Be skeptical of anyone who promises TT will fix all of the above.
If your testosterone normalizes but symptoms persist, that’s actually useful information — it means something else is driving them. A good doctor won’t just stop there; they’ll keep investigating.
Can You Raise Testosterone Without Therapy?
Yes — and for many men, lifestyle changes are the right first step.
Weight loss and regular physical activity can meaningfully raise testosterone levels, particularly in men whose Low-T is tied to obesity or metabolic syndrome. Before jumping to hormone therapy, it’s worth asking whether improving these fundamentals might move the needle on its own.
Questions Worth Asking Your Doctor
Going into an appointment about something this personal can feel awkward. Having a few specific questions ready helps. Consider asking:
-
What tests do I need, and will I need to repeat them?
-
Does my Low-T affect my fertility — and will TT help or hurt that?
-
Which delivery method makes the most sense for my lifestyle?
-
Given my health history, what are my actual cardiovascular risks on TT?
-
If my levels normalize and I still feel bad, what’s the next step?
-
Are there lifestyle changes I should try before or alongside therapy?
The Bottom Line
Low testosterone is a real, diagnosable condition — not just an excuse for feeling run-down, and not something to self-diagnose from an ad. If you’re experiencing a combination of symptoms that feel like a change from your baseline, get tested. The blood work is straightforward, and the answers it gives you are worth having.
Treatment, when genuinely needed, can make a real difference. But it works best when it’s part of a broader conversation about your health — not a standalone fix pulled off the shelf.
This article is for informational purposes only. Always consult a licensed healthcare provider before beginning, changing, or stopping any medical treatment.